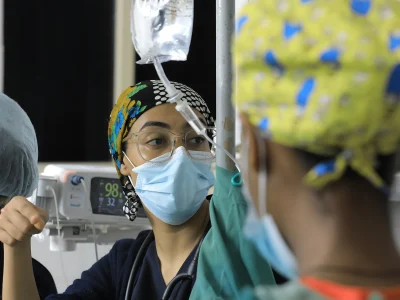
After sixteen years in the operating theatre, I find myself searching for the most powerful way to share my journey. Whether I use words, music, or advocacy, my message rings clear: SAFE SURGERY SAVES LIVES. Even the smallest actions can spark profound change, while overlooking them can put patients in real danger.
This challenge struck me deeply as I witnessed patient after patient suffer from unsafe surgical practices, and as I faced these realities firsthand.
During an open thoracotomy for a right total pneumonectomy, our final count revealed a missing peanut. Despite searching the operating room and surgical field, we could not locate it. Fortunately, the peanut was X-ray-detectable, and with the help of a mobile X-ray unit, we found and removed it near the spine after three hours. The patient became unstable, and the anesthesia team was under significant stress, but managed to transfer the patient to the ICU. About seven days later, the patient developed a surgical site infection and required multiple returns to the operating theatre for chest wall washouts. The team felt deep guilt, knowing the extended search had put the patient at risk.
Joining Lifebox felt like a dream realized. I had the privilege of coordinating a program that improved surgical safety and transformed team collaboration.
I remember one facility where gauze count compliance was a mere 6%. Through training on the WHO Surgical Safety Checklist, the team took a hard look at their habits, tailored the checklist to fit their reality, and pledged to uphold new standards. By the program’s end, compliance soared to 100%. This simple shift proved that real change begins when we choose to act.

During implementation, we zeroed in on six vital perioperative steps: using the WHO Surgical Safety Checklist, preparing skin, ensuring instrument and linen sterility, counting gauze, and giving antibiotics at the right times. We tracked our progress, reviewed quality every two weeks, shared feedback each month, and celebrated every small victory. Watching nurses, surgeons, and anesthetists take pride in these changes became one of the greatest rewards of my career.
I often think about how Clean Cut reached far beyond checklists and protocols. It built a culture where accountability and open communication thrived, empowering those who are often unheard, like the scrub nurse who spoke up about missing counts or the CSSD attendant who pointed out missing sterility indicators in surgical sets.

The impact was evident not only in reduced infection rates and improved compliance but also in personal stories. Previously, I would begin night shifts in the post-cesarean section ward by administering antibiotics to all mothers, often past midnight. Now, only two mothers receive antibiotics, each with clear indications. This change has allowed me to focus on other important tasks and has reduced the risk of antibiotic resistance for our patients.
Now that the work is done, I look back with great pride. Clean Cut and antibiotic stewardship were more than just programs; they sparked a new way of thinking. Together, we built systems that safeguard patients, unite teams, and stand up to the silent danger of antimicrobial resistance.
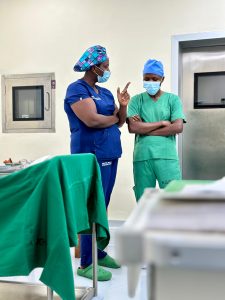
In Rwanda, we have demonstrated that safe surgery is possible even in resource-limited settings. I am confident that the lessons from this journey will continue to spread across hospitals, districts, and borders.
About Roda
Roda Uwayesu is a theatre nurse and public health professional with 16 years of experience in surgical care. She currently serves as Lifebox’s Program Coordinator in Rwanda and is pursuing a Master of Public Health.